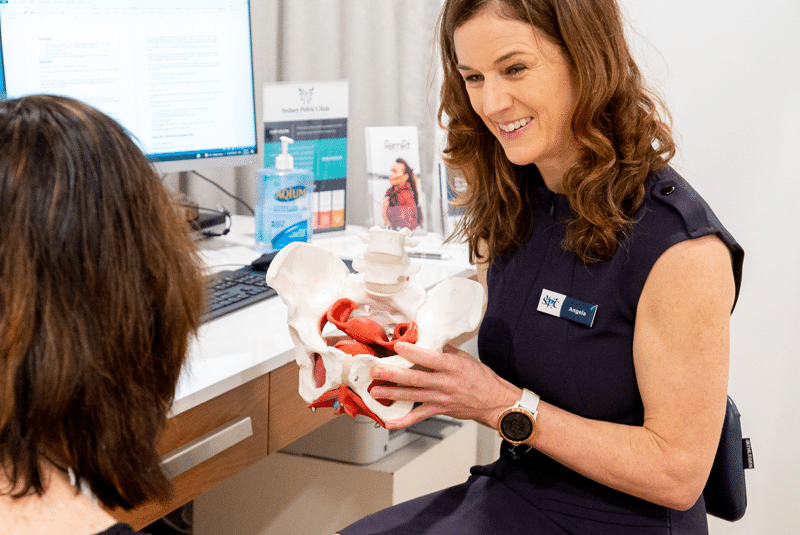
Pelvic pain is a common and often debilitating condition that affects men and women of all ages. Understanding the causes and treatment options can help you to gain some control over your pain, learn how to manage it and achieve relief.
Pelvic pain is common in Australians, affecting 20% of women and around 8% of men (Pain Australia). It commonly presents as a result of an injury, infection or trauma but in some, there may not be a particular inciting event – it might just come on over time, seemingly out of nowhere.
If pain is unmanaged in the early stages, it can go on to become persistent pelvic pain (PPP), which is any pain in the pelvic region that lasts for greater than three months. (For more information on defining pain, see www.continence.org.au). Many people who experience PPP will have a long journey through testing that all comes back ‘normal,’ so it’s common to feel lost in the medical system without answers after being treated with medication that helps for a short time, or not at all.

Image Source: istockphoto.com
People experience persistent pelvic pain in varying ways- different bodies will respond differently to a system that is essentially trying to tell you “something is wrong”, even if there is no tissue damage. Common presentations of pain include genital pain without trigger, pain during or after orgasm, difficulty or discomfort with holding or emptying your bowels or bladder, or a combination of all of the above. For more information on manifestations of pain, have a read of the following articles on Bladder Pain Syndrome and Pudendal Neuralgia:
Persistent pain can be complex in that it is influenced by biological factors such as muscle weakness or tension, (see SPC article – Overactive Pelvic Floor Muscles) but it is also largely influenced by emotions that send your nervous system into fight or flight, like stress. Over time, the mechanism of persistent pain becomes driven by our nervous system and the way our bodies perceive sensation as a threat.

Image Source: istockphoto.com
The good news is that pelvic physiotherapy can help!
Your physio is uniquely positioned to unpack the complexity of pelvic pain by assessing all of the factors that contribute to your pain, and help you to build a toolkit to modify the elements that can mitigate pain. Persistent pain happens at the intersection of the biological (physical), social (lifestyle) and psychological (nervous system) and so addressing each of these elements is necessary for a complete resolution of symptoms.
Our physiotherapists can: teach you about what is driving your pain, help you identify patterns and regulate your nervous system with achievable homework, release tight muscles that often significantly contribute to your pain experience, facilitate exercise that doesn’t flare your symptoms and help you plan for unavoidable triggers so that you are able to manage independently. We also help you to address the flow-on effects of pain, like poor sleep, and will refer you on to trusted therapists as needed, to help you to manage the emotional impact of your pain. We can add modalities such as TENS and shockwave to ‘rewire’ how your body perceives sensation and lower the threat response to sensation so that your pain comes under control.
With good management you can gain control over your pelvic pain to achieve relief, return to your normal life and prevent a recurrence of your symptoms. Moments of pain are a sign of a working nervous system, but persistent pelvic pain does not have to be an ongoing part of your life.