GENERAL PHYSIO CONDITIONS
At Sydney Pelvic Clinic, our approach to general and sports physiotherapy is integrated and individualised. We seek the core driver of the problem, then use innovative and effective evidence based therapy, including soft tissue and joint mobilisation, muscle energy techniques and dry needle therapy combined with education and specific exercise rehabilitation to achieve optimal results.
We create awareness and seek change around non-optimal posture and movement patterns. We optimise function and performance through correct strength and stability training. Ultimately we want you feeling good in your body and doing all the things you love doing!

SPC Physiotherapy Team
CONDITIONS WE TREAT
HEADACHES
NECK
JAW
SHOULDER & ELBOW
WRIST & HAND
RIBS & THORACIC SPINE
KNEE & SHIN
ANKLE & FOOT
Getting Started
STEP ONE

Complete Assessment
Your qualified physiotherapist will begin by assessing your symptoms or injury. This includes a thorough review of your medical history, a full physical assessment, and a thorough evaluation of your symptoms and the effect on your quality of life.
STEP TWO
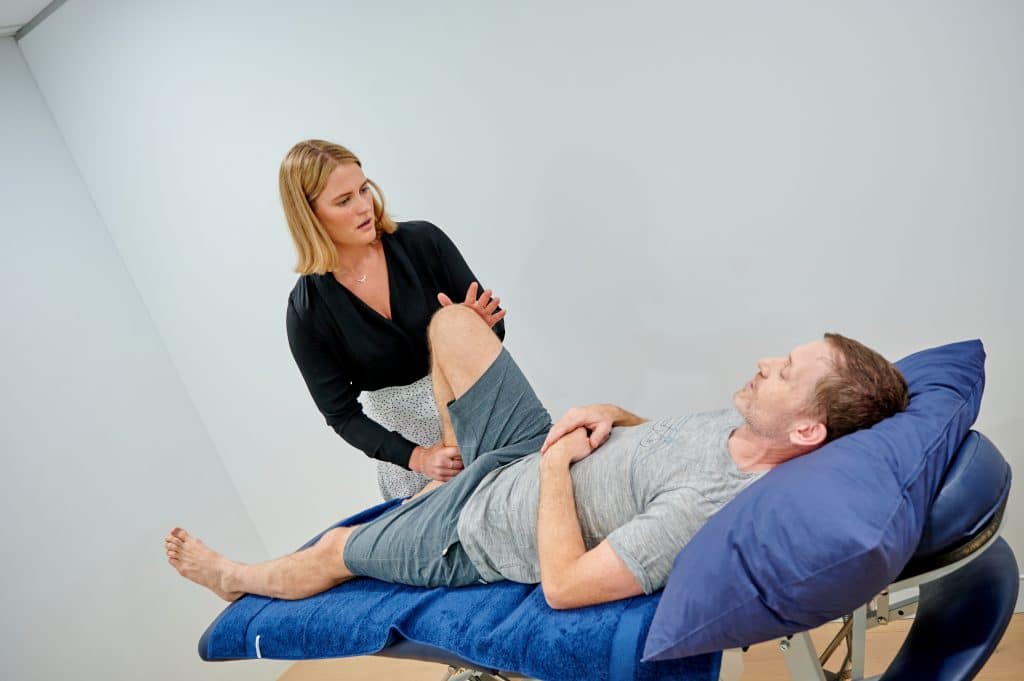
Diagnosis & Explanation
Once the cause of your pain or condition has been diagnosed, your physiotherapist will discuss the findings with you, as well as explaining treatment options and expected outcomes. We combine our holistic, integrated approach with cutting-edge technology to achieve the best possible health outcomes.
STEP THREE

Treatment & Management
Your physiotherapist will tailor an individual treatment plan, which may include one or more of the following; evidence-based manual therapy, strengthening exercises or specific exercise rehabilitation, education, mindfulness techniques, and home management plans for ongoing treatment.
